Contents
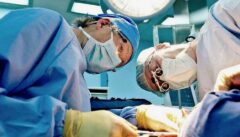
Shortage Of Oral & Maxillofacial Surgeons
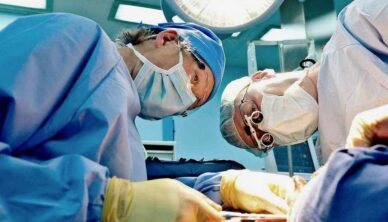
A 2023 study of maxillofacial care in Scotland found that many patients were waiting up to a year for surgical treatment, almost double the time taken 5 years earlier.
Although cancer patients were given a degree of priority, delays could include treatment for cancers, head and neck trauma, cleft lip surgery, or acute dental work.
Where the need was classified as cosmetic, even though the patient may not feel that way, there could see the longest delays. Or more often be given a date, only for this to be cancelled.
Useful insight for Scottish health officials to consider, although there is no wish to suggest they are alone. The issues they face can be seen across the UK.
An Acknowledged Deficit
In 2022, the British Journal of Oral and Maxillofacial Surgery published research on the shortage of consultants in their field. Unfilled consultant posts in mainland Britain stood at 13%, 20% in Northern Ireland.
A number of practical reasons were suggested, pension pressures and tax changes, recruitment, amendments in job plans which restrict the number of sessions.
Concerns for the future were also mentioned, the current average age of oral & maxillofacial consultants was put at 52.7 years, with 23% of consultants above the normal retirement age.
The eventual loss of senior staff will further reduce the capacity to treat oral & maxillofacial disorders, or injuries. At a time when we already struggle to cope.
Causes and Cures
A prime cause is hard to work round. Maxillofacial surgeons need to be fully qualified in medicine, dentistry and core surgical skills.
Other training requirements will have taken a number of years, more if they sub specialise. Acquiring suitable knowledge can take half a working lifetime.
Finding the right people, who are prepared to give that level of commitment is not easy. By the time they are fully qualified, maxillofacial consultants may have twenty years or less to practice before retirement.
Few professions mirror this situation, which is being heightened by an increasing number of consultants choosing to work part time, a reflection of the pressure they feel.
Eliminating downsides and encouraging more consultants to work longer hours would help, along with increasing trainee numbers and the number of consultant posts. Actively retaining senior surgeons makes sense.
Looking To The Future
The recent past has not helped, not least the backlog of care created by the Covid-19 pandemic, or staff shortages following Brexit.
Both added pressure to health services but also highlighted what already existed. A significant gap in the UK between workforce capacity and clinical demand.
Developing technology will ultimately help to relieve certain pressures but we can not change the prime cause mentioned. Maxillofacial consultants need the skills and experience to provide good treatment.
Producing more will only come from appropriate planning, funding, selection and encouragement. Offering these is not beyond us, simply a case of having the will and insight.
We are pleased to offer high quality maxillofacial & oral surgery, yet will be equally pleased when this can be available to more of the UK’s population.
21 September 2024